Capstone believes the applied behavior analysis (ABA) Medicaid benefit remains structurally sound despite a near-term decline in provider reimbursement rates. Federal mandates create a durable demand floor, and proposed rate cuts are intended to align with the national average. As the market resets, ABA operators with diversified state exposure and rates near the national average are poised to benefit as the reimbursement environment stabilizes.
- ABA therapy for individuals under 21 with autism spectrum disorders (ASD) was granted Medicaid coverage in 2014, making it a relatively new benefit. As a result, ABA lacks a federal benchmark, with states setting the reimbursement rates. The rates are not standardized, creating wide variation in provider reimbursement and a rapid rise in state spending. We examine trends across three states that have dominated ABA fraud headlines: Indiana, Minnesota, and Nebraska.
- Among the states we analyzed, Indiana and Nebraska introduced recent rate cuts for ABA providers. Capstone analysis shows the new rates are better aligned with the national average. Of note, the new rates remain above the national average, limiting the impact on compliant providers.
- The scrutiny of fraudulent provider behaviors offers compliant ABA operators a tailwind, with an opportunity to build market share as outliers exit Medicaid markets.
ABA under Medicaid is a relatively new benefit, which explains the lack of standardized rates
States are required to cover ABA therapy under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) requirement, which mandates Medicaid programs to provide comprehensive and medically necessary services for individuals under 21 who are eligible for Medicaid. As a mandate under EPSDT, ABA is a required benefit in all states, with any changes to the mandate requiring congressional action. States will continue to be required not only to cover ABA but also to provide sufficient reimbursement to providers to ensure adequate access to Medicaid enrollees.
Although the EPSDT requirement has been in place since 1967, the Centers for Medicare and Medicaid Services (CMS) clarified the inclusion of ABA therapy in 2014, making the benefit for individuals with autism relatively new. In the 2014 announcement, CMS reinforced that coverage of ASD services under Medicaid is protected under the requirements for children’s benefits.
Most states formally announced this Medicaid coverage in 2014, while others codified it later, as CMS did not provide a timeline to establish coverage. For example, North Carolina was one of the earliest adopters in 2014, while Texas did not formally announce ABA Medicaid coverage until 2022. Under EPSDT, states are not only mandated to cover medically necessary services for children but also to ensure that provider reimbursement rates are sufficient to ensure adequate access to care.
Given that ABA is a relatively new Medicaid benefit, states have historically not standardized ABA therapy utilization management techniques and reimbursement methodologies. Moreover, there are no Medicare rate benchmarks for ABA, and as a newer benefit, states could not easily benchmark rates to those of neighboring states. This led to the lack of a standardized fee schedule in the industry, while some states such as Indiana relied on a percentage of billed charges reimbursement methodology to reimburse ABA providers. Reimbursing through a percentage of provider-billed charges resulted in significant variations in reimbursement across providers for the same service, with a handful of providers submitting inflated claims, substantially increasing overall state spending for ABA (see Exhibit 1).
Exhibit 1: Growth in ABA Spending Over Time, in $ millions
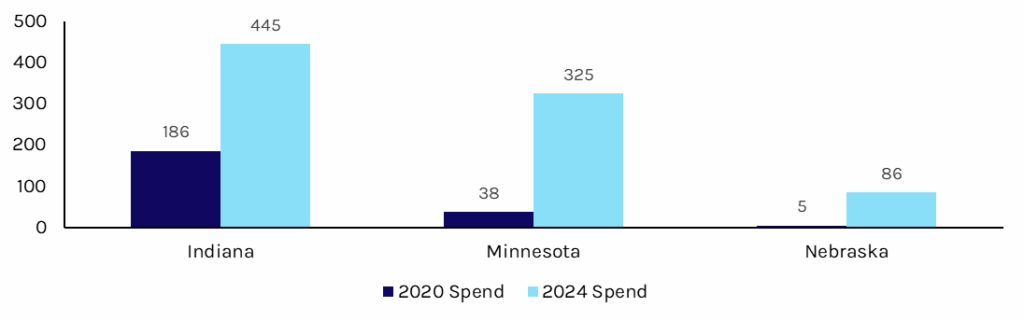
Source: Indiana Family and Social Services Administration, Minnesota Special Reviews Division, Nebraska Department of Health and Human Services
States have introduced provider reimbursement cuts to align rates with the national average
In efforts to standardize rates to those of neighboring states and the national average, Indiana and Nebraska have introduced rate cuts, hampering Medicaid provider reimbursement. Capstone analysis of rates in these select states reveals that state benchmarks are adjusted to better align with the national average BT reimbursement rate of $62.80, based on 2024 data.
Indiana introduced a state-set fee schedule for ABA in 2024, moving away from the original rate methodology that reimbursed 40% of provider-billed charges. The state introduced another rate cut effective April 2026 to better align rates with the national average. Similarly, Nebraska has introduced recent rate cuts in response to rising expenditures, although the new rates remain above the national average (see Exhibit 2).
Exhibit 2: State Medicaid Behavioral Technician (BT) Rate, in $ per hour
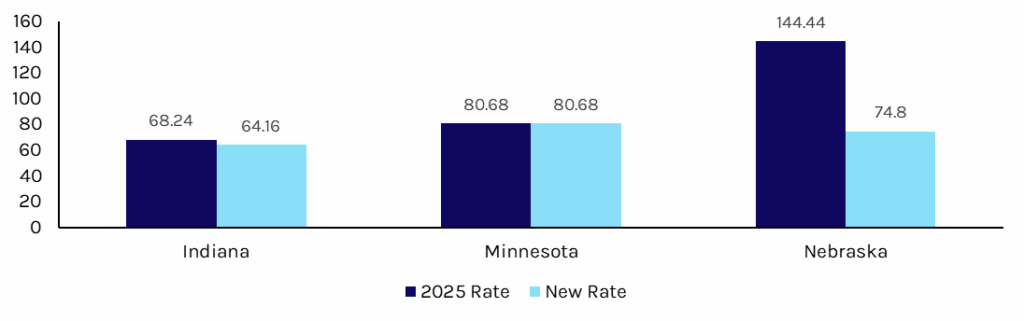
Note: Nebraska’s rate cut was effective in August 2025. Minnesota has not introduced a rate cut.
Source: state Medicaid fee schedules
Headline risk represents some bad actors in the market, not an industry-wide indictment
Capstone believes that state actions tightening utilization and reducing reimbursement rates are largely targeted at bad actors in the market or attempts to reset rates to the national average. Recent state actions do not indicate a widespread sentiment toward the ABA industry overall, as a few bad actors whose billing practices distorted the market have generated much of the negative press surrounding the ABA. Indiana Medicaid serves as a prominent example (see Exhibit 3), with large variations in Medicaid claims during Q1 2023, as the percentage of billed charges methodology resulted in a handful of bad actors that submitted inflated claims to secure high reimbursements. Notably, many providers continued billing at standard rates, resulting in minimal to no impact on rates once the state switched over to a fee schedule.
Indiana’s enforcement response to normalize rates will most likely have a significant impact on providers that have historically submitted outlier rates. For well-run ABA providers with strong compliance infrastructure, this presents a market tailwind and an opportunity to gain market share as the ABA Medicaid benefit remains structurally intact.
Exhibit 3: Indiana Medicaid ABA Paid Claims, in $ per hour
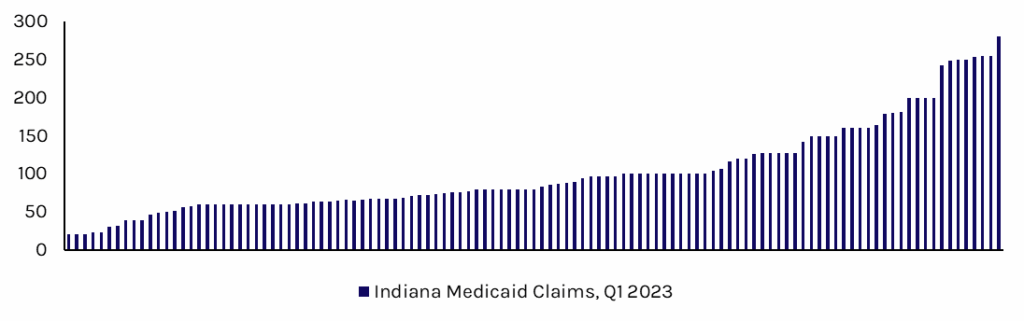
Source: Indiana Family and Social Services Administration
What’s Next
Capstone will continue to track changes impacting the autism industry, including fraud investigations and enforcement timelines, as well as updates to state fee schedules affecting provider reimbursement.
Read more of Capstone’s healthcare coverage:
What Will Vaccine Policy Chaos Cost Payors?
European Digitization Gaps Create Opportunities for Healthcare IT Investment
Making The Case For Cloud Fax Vendors in Healthcare




























